
Tips & Tools
Managing your anxiety
Part One: Naturopathic Approaches to PMS and Mental Health

Have you ever thought of why you feel especially anxious or depressed at around the same time each month? Did you know that your menstrual cycle, and the hormone changes that come along with it, could have a pretty significant effect on your mental health? We commonly group this under a well known abbreviation; PMS, but is there more to it?
We reached out to Dr. Erin TeWinkel, a naturopathic doctor specializing in hormonal and mental health. Since May is Mental Health Awareness Month and Mother’s Day marked the beginning of National Women’s Health Week, it was the perfect time to ask Dr. Erin some questions involving PMS and its connection to mental health. Dr. Erin’s answers will blow your mind with the beneficial awareness that connects your mental health and your menstrual cycle! Part one discusses the various types of PMS and what a Naturopath can do to help you.
Many of us are familiar with PMS, but are there different types of PMS?
Premenstrual Syndrome (PMS) describes a group of symptoms that occur cyclically and improve shortly after menstruation starts.
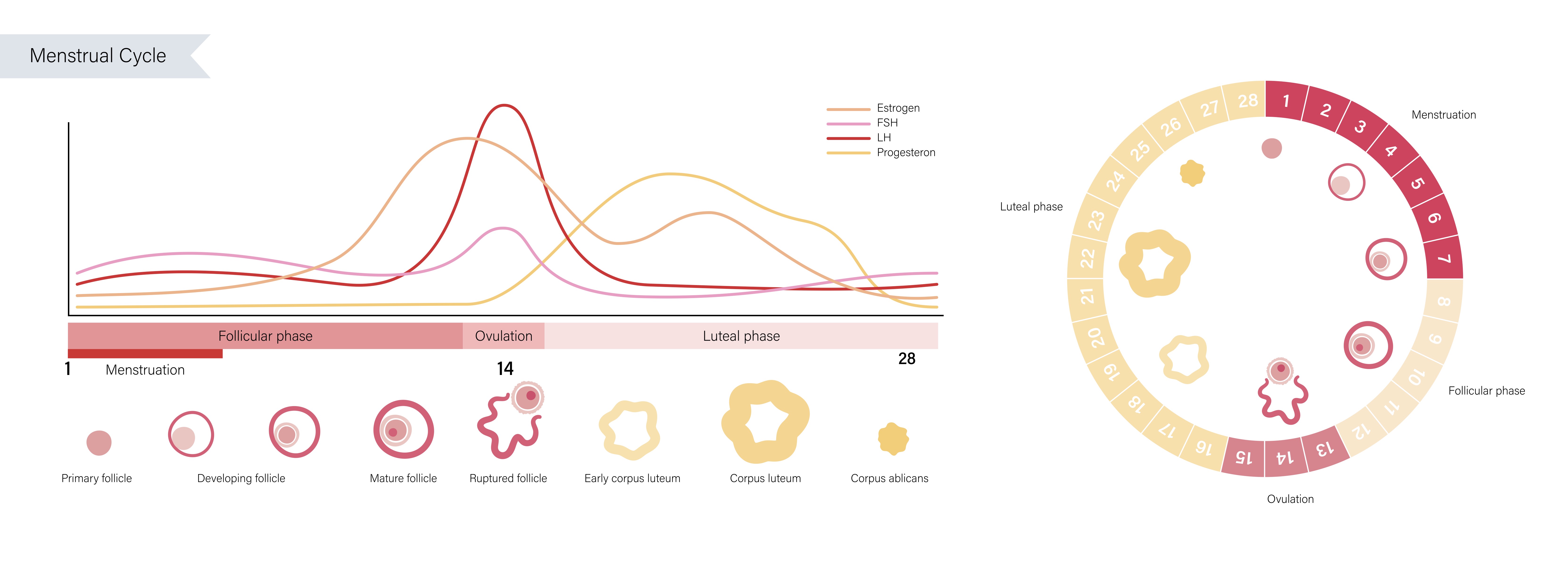
Menstruators are often aware their period is coming from emotional and physical changes that occur in the second half of the menstrual cycle, so after ovulation and before the onset of menstruation. However, if these become extreme or impeding activities of daily living, we often discuss it as a few subtypes:
PMS-D (depression): low mood with lethargy, forgetfulness, and confusion.
PMS-A (anxiety): more sensitive than usual (especially to perceived rejection or criticism), feeling on edge or irritable, feelings of overwhelm
PMS-H (water retention): abdominal bloating, weight gain of over 3 pounds, Breast tenderness/swelling
PMS-C (cravings): increased carbohydrate cravings, a general increase in appetite, fatigue, and headaches.
PMDD: this is PMS-D but much more debilitating - right after ovulation until the first day of menses, there is extreme depression and even as extreme as thoughts of suicide.
Premenstrual dysphoric disorder (PMDD) is different from depression or anxiety that someone already has that can be worsened during the luteal phase. A person experiencing PMDD often feels great the other 2 weeks of the month, and then as soon as they ovulate, depressive symptoms appear and are relieved as soon as menstruation starts.

A few things to point out:
It's normal to feel a bit more tired and hungry the week before and during your period - shedding the uterine lining is metabolically taxing, and it's normal for your hunger levels to ebb and flow throughout your cycle.
Is there specific testing that a Naturopath could help determine why I am experiencing these mental health slumps at certain times of the month?
The first step is data collection, tracking your period and the symptoms you experience! We can learn a lot just from your experience. Things to track: length of cycle (from Day 1 (first day of bleeding) to the next day), how many days of bleeding, signs of ovulation (cervical fluid changes), plus any and all symptoms with their severity and on what day they happen. Often I encourage patients to use a tracking app plus the DRSP (Daily Record of Severity of Problems)
From there, we would decide if further testing is necessary to help determine a diagnosis. Usually, it is serum hormones: Day 3 estradiol, progesterone, FSH and LH, plus Day 21 progesterone. Depending on other symptoms, we may test fasting insulin, iron, HB1Ac, Vitamin D, and testosterone. We use these to rule in or rule out other menstrually related diagnoses. But there is no actual blood work or test that proves or disproves PMS - the diagnosis is based on the person's experience and by showing that the symptoms happen cyclically with their cycle by tracking.
Are there therapies you offer to help regulate my hormones and support my mental health?
PMS is not a dysregulation of hormones - it's a stress response to our hormones changing - which they are supposed to do. Some menstruators experience that shift more intensely than others. Oftentimes when there is anxiety or depression already, those symptoms can feel worse during the luteal phase of a menstruator’s cycle. Supporting your mental health overall will support your PMS. The best current research for therapies to support anxiety and depression are: (these should be used under the direction of a healthcare practitioner) St. John’s wort, saffron, lavender, GABA, theanine, Vit D, fish oil, plus correcting any nutritional deficiencies, like iron or B12.
But for PMS specifically, the data we have that can support is:
Vitamin D - getting your Vit D levels checked and into optimal range improves the PMS experience.
Calcium - calcium supplementation at the correct dosing shows benefit in reducing PMS symptoms.
Remember, this does not constitute medical advice and adding in any supplements or medications should always be discussed with your healthcare practitioner (HCP).
Plus, click here to see part two of the Naturopathic Approaches to PMS and Mental Health blog for lifestyle habits.
Overall, a naturopathic doctor can do so many things to help guide and support our hormones, and this can also be impactful when it comes to mental health. Naturopaths will analyze the data, administer tests that are needed, and give further recommendations, including supplementation.
 |
Dr. Erin TeWinkel, ND Instagram: @drtewinkel Website: www.drtewinkelnd.com |
References:
Abdi, F., Ozgoli, G., & Rahnemaie, F. S. (2019). A systematic review of the role of vitamin D and calcium in premenstrual syndrome. Obstetrics & Gynecology Science, 62(2), 73–86. https://doi.org/10.5468/ogs.2019.62.2.73
Arab, A., Rafie, N., Askari, G., & Taghiabadi, M. (2020). Beneficial Role of Calcium in Premenstrual Syndrome: A Systematic Review of Current Literature. International Journal of Preventive Medicine, 11, 156. https://doi.org/10.4103/ijpvm.IJPVM_243_19
Bahrami, A., Avan, A., Sadeghnia, H. R., Esmaeili, H., Tayefi, M., Ghasemi, F., Nejati Salehkhani, F., Arabpour-Dahoue, M., Rastgar-Moghadam, A., Ferns, G. A., Bahrami-Taghanaki, H., & GhayourMobarhan, M. (2018). High dose vitamin D supplementation can improve menstrual problems, dysmenorrhea, and premenstrual syndrome in adolescents. Gynecological Endocrinology: The Official Journal of the International Society of Gynecological Endocrinology, 34(8), 659–663. https://doi.org/10.1080/09513590.2017.1423466
Behboudi-Gandevani, S., Hariri, F.-Z., & Moghaddam-Banaem, L. (2017). The effect of omega 3 fatty acid supplementation on premenstrual syndrome and health-related quality of life: A randomized clinical trial. Journal of Psychosomatic Obstetrics and Gynaecology, 1–7. https://doi.org/10.1080/0167482X.2017.1348496
Erman Esnafoglu 1, Deniz Deniz Ozturan. The relationship of severity of depression with homocysteine, folate, vitamin B12, and vitamin D levels in children and adolescents. Child Adolesc Ment Health 2020 Nov;25(4):249-255. Epub 2020 Apr 18.
Joseph Firth 1, Wolfgang Marx, Sarah Dash, Rebekah Carney, Scott B Teasdale, Marco Solmi, Brendon Stubbs, Felipe B Schuch, André F Carvalho, Felice Jacka, Jerome SarrisPsychosom. The Effects of Dietary Improvement on Symptoms of Depression and Anxiety: A Meta-Analysis of Randomized Controlled Trials. Med2019 Apr;81(3):265-280.
L T Møllehave 1, T Skaaby 1, K S Simonsen 1, B H Thuesen 1, E L Mortensen 2 3, C H Sandholt 4, O Pedersen 4, N Grarup 4, T Hansen 4, A Linneberg 1 3 5. Association studies of genetic scores of serum vitamin B12 and folate levels with symptoms of depression and anxiety in two danish population studies. Eur J Clin Nutr2017 Sep;71(9):1054-1060.doi: 10.1038/ejcn.2017.97. Epub 2017 Jun 28.
Siddiqui MJ, Saleh MSM, Basharuddin SNBB, Zamri SHB, Mohd Najib MHB, Che Ibrahim MZB, et al. Saffron (Crocus sativus L.): As an Antidepressant. J Pharm Bioallied Sci. 2018;10(4):173–80.
Skovlund CW, Morch LS, Kessing LV, Lidegaard O. Association of Hormonal Contraception with Depression. JAMA Psychiatry. 2016 Nov 1;73(11):1154-1162 PubMed PMID: 27680324
Szegedi A, Kohnen R, Dienel A, Kieser M. Acute treatment of moderate to severe depression with Hypericum extract WS 5570 (st john's wort): Randomised controlled double blind non-inferiority trial versus Paroxetine. BMJ. 2005;330(7490):503
- All
-
29 Nutrition
Nutrition
- 73 Mindfulness and Relaxation
- 27 Student Life
- 8 Exercise
- 51 Treatments & Therapies
- Anxiety Resources

Don't see what you're looking for? Send us an email!
©Copyright 2024 Cam’s Kids powered by Kids Help Phone
Not-for-Profit Organization. B/N: 921508-5
Thanks for visiting Cam's Kids. Please remember...
Cam's Kids is not a service provider.
If you are in crisis, please call 911 or go to your nearest emergency department. For free, confidential counselling, contact Good2Talk or Kids Help Phone.
Post-secondary students: find your local crisis resource here.

